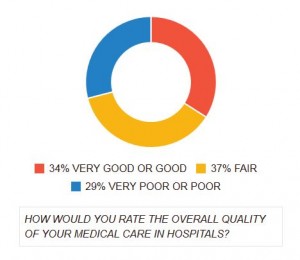
Over 1250 acute or chronic pain patients participated in an online survey by Pain News Network and the International Pain Foundation that focused on hospital pain care. Based on the results obtained, many pain patients felt that the treatment they received from a hospital was far less than ideal. As one pain patient stated, “It’s so bad that I will not seek treatment in an ER or hospital unless I really feel like my life is in jeopardy. They do not get it, they do not listen, and they do not care.” Another individual wrote, “I refuse to go to ER. It will end up killing me because I know how sick I am, but I would rather die than deal with ignorant, condescending doctors and nurses.” To read more about this study’s findings, click here.




 Negative relationships can exist between physicians and their presence can impact patient care. As Dr. Karthikesan explains, “The doctor-patient relationship paradigm depends closely on the doctor-doctor relationship. Bad and damaging cultures foster a hostile atmosphere that erodes trust, tarnishes good communication and promotes disrespect within the medical community. The role doctors play in harming each other ubiquitously affects the patient’s care, however unintentionally. The question becomes, how can the relationship between physicians be improved or as Karthikesan asks, “So what went wrong in the noblest of professions and how do we fix it?”
Negative relationships can exist between physicians and their presence can impact patient care. As Dr. Karthikesan explains, “The doctor-patient relationship paradigm depends closely on the doctor-doctor relationship. Bad and damaging cultures foster a hostile atmosphere that erodes trust, tarnishes good communication and promotes disrespect within the medical community. The role doctors play in harming each other ubiquitously affects the patient’s care, however unintentionally. The question becomes, how can the relationship between physicians be improved or as Karthikesan asks, “So what went wrong in the noblest of professions and how do we fix it?”