 Family Presence is becoming an important topic in Alberta’s healthcare system. As such, we have added a Family Presence area to our website. There you will find some new material that is hot off the press! Click here if you are looking for Family Presence tips, conversation starters and more…
Family Presence is becoming an important topic in Alberta’s healthcare system. As such, we have added a Family Presence area to our website. There you will find some new material that is hot off the press! Click here if you are looking for Family Presence tips, conversation starters and more…
Tag Archives: advocacy
You Are Invited…
Pts4Chg is presenting at the International Institute for Patient and Family Centred Care (IPFCC) conference that is occurring from July 25-27th. As part of the presentation, a Twitter exchange will be taking place. Please consider joining us in the Twittersphere to converse with conference delegates, share ideas and have fun. 
Date: Tuesday, July 26, 2016
Time: 11:15 a.m. EST
Location: In the Twittersphere at #Pts4ChgNYC
Helping Oneself and Others

In an online post, Sheila, a member of the Pts4Chg community, raises an important topic. How does one obtain assistance for oneself or others when it comes to health care? How does one
tactfully get help for yourself or a loved one, or even possibly someone we don’t know who is in the hospital and we see that he/she is not getting the care that the Dr. prescribed, such as meds being missed or denied, patient not being fed, etc. Sadly, only those who have a loved one who comes to visit, will get these issues fixed, but I have seen (too many times) meals delivered to people without a loved one there to feed them, which were just picked up and taken away when the dietitians came back to collect trays, no one to feed those who are the most sick and alone or help them get the care the Dr. prescribed. In my local hospital, those with visitors get the most care because then there are ‘witnesses’ to what did or did not happen. The ones who are alone are in a dangerously negligent position.
Any comments and suggestions relating to this topic are welcome.
Seeking Your Input on the Nursing Home Legislation
Interested in health care and want to make a difference?
If you are interested in health-care services and want to make a difference, here is an opportunity that you may wish to explore. Please note that the deadline for applications was May 18, 2016, but has been extended.
What Will You Do?
Rare Disease Day is tomorrow, February 29th. What will you do to recognize the day? #RDD2016 https://t.co/Bgx7xC3iFl
— Patients 4 Change (@Pts4Chg) February 28, 2016
“Patient organisations in Canada have engaged in Rare Disease Day since its first year in 2008, arranging gala dinners and exchanges between researchers and patients, as well as regional events across Canada.
The undisputed highlight of the 2015 event was the transformation of the iconic CN Tower with blue lighting to celebrate Rare Disease Day, as was done in 2014 as well. Elsewhere in Canada local communities got together for bake sales, dinners, and research forums.
The Canadian National Alliance, the Canadian Organization for Rare Disorders (CORD), serves as the voice for the estimated 1 in 12 Canadians affected by a rare disease. They can be contacted directly to help you find a patient organisation locally which may have more information about a specific rare disease or disorder.” http://www.rarediseaseday.org/country/ca/canadae-disease-day)
The following pictures are of Melanie, an individual who suffers from the rare disease – gastroparesis.
(Pictures were submitted by D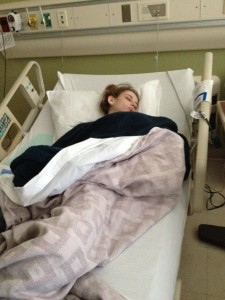 eborah, February 28, 2016.)
eborah, February 28, 2016.)
As Melanie’s mother, Deborah, states, “That’s what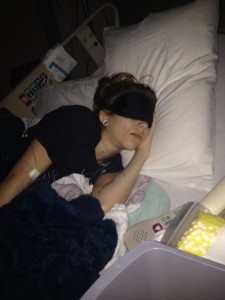 I have to look forward to every month for three days.”
I have to look forward to every month for three days.”
Stop Kicking the Cat
According to David Gilbert, author of the Future Patient Blog, there is an opportunity to make radical changes in the area of healthcare. This requires that people, including patients and the general public, are given their rightful responsibilities and accountability. Gilbert maintains that patients can help to improve the healthcare system. However, for this to occur, the manner in which patients are viewed, treated and the understanding and approach of patient engagement must be changed.
We do not live in normal healthcare times of course. The pressures on healthcare delivery in a changing society seem not be accompanied by any coherent vision of how to cope with those changes. The desperation for a new sense of order and the tendency to kick the cat seems actually to be increasing. Though national agencies may talk of letting go, the sense of grip and pressure felt at a local level is intense. Polarisation and power battles are inevitable.
I believe that patients can help.
Patients can be true partners for improvement and change. They can help identify what matters, rethink problems, generate solutions, model better relationships, promote better decisions and improve practice. (see, The Seven Things That Patients Bring). But, at the moment we are all hamstrung by bad habits.
The way we think about patients’ contributions is stuck in a time warp, our mindset constrained by an outmoded view of what patients can bring (or cannot). Moreover, the way we do patient and public engagement is not working – it fails to have any real impact because it is outmoded and unfit for purpose. In part, it was never designed to bring real change, but to buffer it and maintain the status quo. Now, if we really want solutions to our current healthcare challenges, this all needs to change.
Click here to read the article.

