If you have not yet put Alpha House’s Encampment Team and DOAP Team’s numbers in your phone, please do so now. 403 805 7388 and 403 998 7388 respectively. The coming cold snap will be especially serious for individuals experiencing homelessness #SeeSomethingSaySomething pic.twitter.com/OGGKq6BMaU
— Alpha House Calgary (@alphahouseyyc) January 8, 2020
Tag Archives: caring
Sandra’s Words
 Have you read Sandra’s very powerful and heartfelt message that she wrote on December 5th, 2019? If not, you may wish to do so below. https://m.facebook.com/story.php?story_fbid=1148512898813667&id=100009649036230&ref=bookmarks
Have you read Sandra’s very powerful and heartfelt message that she wrote on December 5th, 2019? If not, you may wish to do so below. https://m.facebook.com/story.php?story_fbid=1148512898813667&id=100009649036230&ref=bookmarks A Wish Granted

Oft times, corporations are seemingly so focused on their bottom line that they forget about the human side of their business and indeed the people whom they are working with and for. Fortunately, such was not the case for Disney, who granted five-year-old Ellery a special wish.
Click here to read the full story.
A video worth watching
PHSA's #IAmYourNurse campaign has reached more than 1.25 million people, and now it's won three @IABC Silver Leaf Awards, for Employee Engagement, HR & Benefits Communication and Audio Visual. Congrats to all involved, especially @junipil and the nurses who inspired the video! pic.twitter.com/4CuEZXeNTT
— Prov Health Services (@PHSAofBC) October 29, 2019
A Hospital Halloween
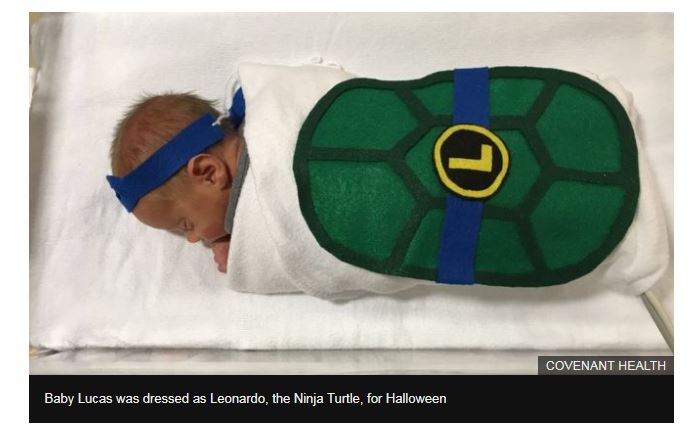
A Canadian hospital is helping make the hospital experience less spooky for parents of sick or premature newborns.
Yesterday, I was talking to some friends whose son is in the Alberta Children’s Hospital. According to J.W., they had spent over $60.00 for a Halloween costume for their two-year-old son, M.W. Unfortunately, due to a medical issue that arose on October 29th, the costume had not been worn and remains in its original bag.
Hearing this, I was reminded of an initiative that had been started by two nurses on a neonatal unit. The end result saw babies wearing handmade felt Halloween costumes at a hospital in Edmonton. Click here to read the story.
A Must Read
A definite "must read" and time well spent. "'I am mine': This is what Alzheimer's is like at 4" #alzheimers #healthcare #familypresence #patientexperience https://t.co/4Vedw0aPTC
— Patients 4 Change (@Pts4Chg) September 19, 2018
Become a Patient Advocate
-
Do you reside in the Edmonton area?
-
Are you a caring, empathetic, compassionate individual who is looking for a way to make a difference in the lives of others?
If your answer to the above questions is “Yes,” the Open Arms Patient Advocacy society is looking for you. Click here to read more about this exciting opportunity.
Storytelling and Healthcare?

Have you heard about storytelling? Are you interested in learning how storytelling can affect healthcare? If you answered “Yes” to both of these questions and if you are going to be in Edmonton or area on January 29, 2018, here is something you may want to check out.
Out in the Streets

Dr. Jeff Turnbull gets a hug from Shelley, a client, after she gave him a Christmas card, at the Temporary Enhanced Shelter Program at the Shepherds of Good Hope in Ottawa’s Lowertown neighbourhood, Thursday, Dec. 14, 2017. (Photograph by Justin Tang)
Have you heard of Dr. Jeffrey Turnbull? If not, reading the following will give you a sense of who he is and the important work he is doing.
“At 9:30 a.m. on a bitingly cold early-winter morning, Jeffrey Turnbull is preparing to head out on rounds. From a second-floor window in the ramshackle offices of Ottawa Inner City Health, the Peace Tower is visible in the distance, but Turnbull gestures out over the nearer, nondescript rooftops of Lowertown, describing the long-established homeless shelters there—and the new supervised injection clinic—that he’s about to visit.
A few minutes later, he’s parking his SUV outside the Shepherds of Good Hope, a shelter and soup kitchen, leading a small team that includes a mental health nurse into what they just call “the trailer.” It’s a former construction trailer set up recently behind “the Sheps,” fitted out as a cramped but orderly space where drug addicts can inject themselves with health care workers standing by.
Even on this weekday morning, it’s busy. About 130 addicts used the trailer the previous day. Turnbull has a brief meeting with staff there, then strides next door to a clinic for homeless women…” Click here to read the full article from the Macleans.ca.
What is empathy?
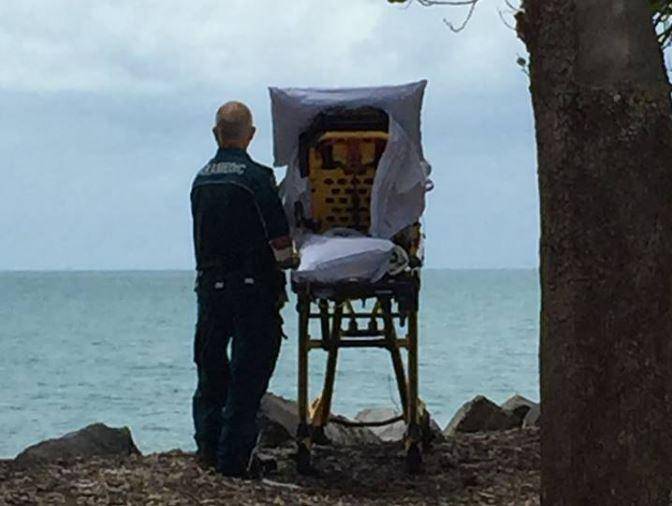
The paramedics who were driving a dying woman to the hospital took a detour, and in so doing fulfilled her final wish.
“Sometimes it is not the drugs/training/skills – sometimes all you need is empathy to make a difference!”
Click here to read this heartwarming story.